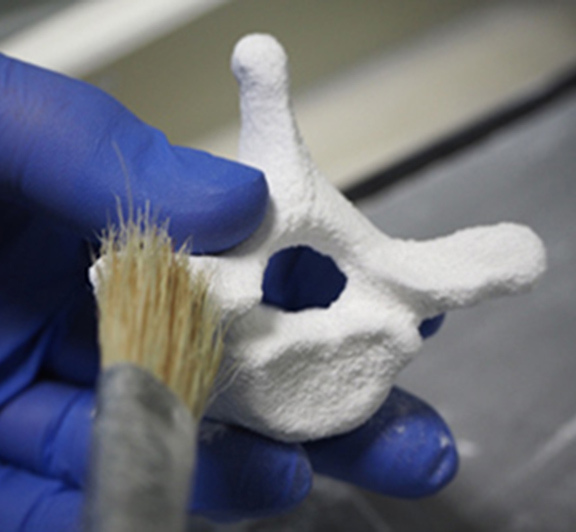
Bioactive Inorganic Scaffolds
The development of inorganic scaffold materials for bone regeneration at FMZ is based on reactive calcium- and magnesium phosphates (CaP and MgP) that set after addition of water under ambient conditions by a dissolution – precipitation reaction. Primary aims are focused on the synthesis and reactivity of the powders, their rheological optimization for injectability, the biological behavior in vitro and in vivo, and the mechanical strength of the resulting ceramics. A current development concerns bioceramics and cements based on magnesium phosphate chemistry. The rationale behind this is the good solubility of MgP phases under in vivo conditions and the fact that Mg2+ is a potent inhibitor of hydroxyapatite crystal growth thereby suppressing unwanted crystallization in vivo. In contrast to implants made of magnesium metal, magnesium phosphate ceramics and cements do not produce hydrogen gas and an alkaline environment during dissolution.